
Get a Free quote

In recent months clinicians and rehabilitation specialists have increasingly highlighted external supports as a practical layer in knee care, especially for people returning to activity after injury or dealing with ongoing joint discomfort. The devices, often called knee stabilizers in consumer and clinical discussions, are being framed not as replacements for treatment but as adjuncts that can improve day-to-day comfort and confidence while other steps in recovery proceed.
Medical teams say these supports work through a mix of mechanical guidance and sensory feedback. That combination can help guide movement patterns, reduce painful pressure on vulnerable joint regions, and offer a controlled environment for tissues that are healing. For patients and active individuals alike, the question has moved from whether a support can be worn to when and how it should be introduced into a rehabilitation plan.
Knee supports are designed to assist the joint without taking aim at a single cure. Their practical roles include:
Those four effects combine to create an environment in which exercise, balance training, and gradual return to activity can be carried out with greater confidence.
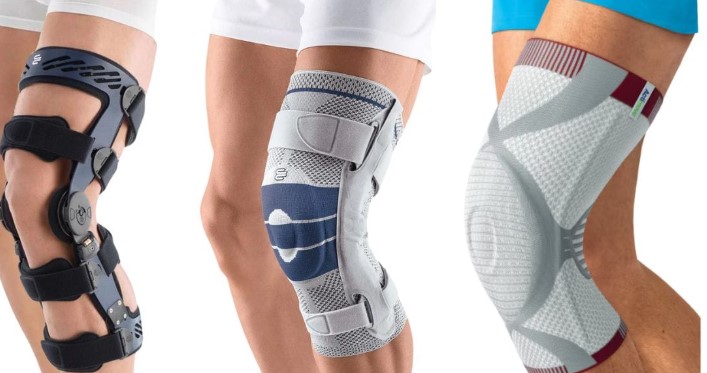
Rehabilitation professionals typically consider several factors before advising a support. A clear benefit is the extra protection given during early return to sport or higher-demand tasks, when tissues are still regaining tensile strength or coordination. For people coping with degenerative joint changes, the device can help reduce pressure on targeted surfaces during walking or stair use, which may ease symptoms enough to allow more consistent physical activity.
Surgeons and physiotherapists often view external supports as a temporary aid in a broader recovery plan. Used alongside progressive strengthening, mobility work, and functional retraining, a support can be a bridge to independent activity rather than a permanent dependency.
There are clear scenarios that require caution. Relying on an external device while neglecting the muscles around the joint can reduce the stimulus those muscles need to rebuild strength and endurance. In cases of severe structural damage, such as a complete rupture of a major ligament, an external device rarely replaces the need for focused medical evaluation and may only play a limited role while definitive care is planned. Finally, comfort and fit matter: an ill-fitting support can cause rubbing, numbness, or altered movement mechanics that create new problems.
| Clinical goal | How an external support helps | When alternative care is likely needed |
|---|---|---|
| Early return after ligament sprain | Limits hazardous directions of motion; adds confidence for gradual activity | Complete ligament rupture or ongoing joint instability on test |
| Joint wear and pain | Redistributes load away from painful area; reduces swelling with compression | Advanced structural loss causing persistent giving way during daily tasks |
| Postoperative protection | Restricts risky movements while tissues heal | When surgical repair or revision is still required to restore stability |
| Activity protection for athletes | Adds a layer of control during training as strength rebuilds | When pain prevents safe participation or there are repeated sudden instability episodes |
A physiotherapist working in outpatient care explains that a support can reduce fear of movement, which in turn reduces guarding and allows better exercise performance. A sports medicine clinician adds that the devices are helpful when used to complement progressive loading — controlled exposure to movement and weight that provokes adaptation without overload. Multiple clinicians stress that any decision to use external support should align with an assessment of strength, coordination, and the specific tissue that was injured.
These steps are aimed at reducing the risk that people become dependent on external support while their musculature and movement patterns remain undertrained.
From a public-health view, practical tools that allow people to remain active while managing symptoms have value. When mild instability or pain would otherwise limit daily movement, appropriate support can enable continued exercise and participation in work or social life. In the sporting realm, measured use during re-introduction to practice can protect healing tissues while skills are rebuilt.
At the population level, however, it is critical that the supports are not presented as a single solution. Without concurrent attention to conditioning and technique, the short-term advantages can be offset by longer-term weakness or compensatory patterns.
Professionals and nonprofessionals alike use a range of terms. The word knee stabilizers appears in both clinical notes and lay discussions; across the conversation, it refers broadly to external devices intended to guide motion and reduce harmful loads. When considering options, focus on how a device performs relative to your goals rather than on labels or claims. Fit, comfort, and a plan for progressive activity matter far more than marketing language.
Emerging guidance from clinicians emphasizes education alongside use. Rather than offering a device as an isolated fix, teams are pairing it with instruction on exercises that target the muscles supporting the knee, strategies to modify activity safely, and criteria for when to reduce reliance on external help. That combined approach aims to preserve the short-term support benefits without allowing underlying deficits to deepen.
For readers weighing whether an external support could help with daily tasks or a supervised return to sport, the key steps are assessment, tailored prescription, and integration with a rehabilitation plan. Used in that way, the supports can offer a practical layer of protection during recovery. People who want to explore this option should consult a clinician who can review their specific situation and suggest an individualized approach; when a device is chosen, clarity about goals and a timeline for progressing exercise are essential. For more background information and resources, see steriger .